Neurological and Neurodevelopmental Disorders
The brain is the most complicated organ
Why is it a problem?
Why is it a problem?
First things first: what are these disorders?
Neurological and neurodevelopmental disorders are dysfunctions in part of the brain or nervous system that result in physical or psychological symptoms that can affect a child’s behaviour, memory, or ability to learn. Common neurological and neurodevelopmental disorders are:
• ADHD (attention deficit hyperactivity disorder)
• Autism
• Brain Tumours
• Traumatic Brain Injury
• Cerebral Palsy
• Dyslexia
• Epilepsy
• Foetal Alcohol Syndrome
• Hydrocephalus
• Migraines
• Motor Neuron Disease
• Multiple Sclerosis (MS)
How do they happen?
Most neurological disorders are present at birth either due to genetic or environmental factors, e.g. spina bifida or hydrocephalus (fluid in the brain) or Foetal Alcohol Syndrome. Disorders that are acquired after birth are rarer and can be caused by serious infections or traumatic injuries.
What is neurological and neurodevelopmental research?
Basic research
Scientists investigate the biology of the brain and nervous system, how they work together and the pathology (nature and cause) of the disease or disorder.
Clinical research
Via lab-based research, scientists and physicians can trial and test new ways of preventing, treating, slowing or curing neurological conditions, e.g. developing new drugs, trying new surgical techniques, gene therapy, immunology or stem cell treatments.
Translational research
Taking the findings from basic science and clinical research in the lab into real-world scenarios and practice.
Did you know?
Approximately 100 children in New Zealand are diagnosed with hydrocephalus each year.
WHAT ARE WE DOING TO HELP?
Here are just some of the research projects we are funding to help improve neurological and neurodevelopmental health for New Zealand kids.
Improving the lives of children with hydrocephalus
Professor Simon Malpas, University of Auckland
Hydrocephalus is an abnormal build-up of fluid around the brain. Approximately 100 paediatric patients in New Zealand are diagnosed with hydrocephalus every year making it the most common paediatric neurosurgical condition.
Professor Malpas and his team have developed a much-needed ‘pressure sensor device’ to let parents and caregivers monitor their child’s brain pressure remotely. The tool will reduce hospitalisations and radiation exposure from CT scans, and greatly relieve the anxiety of parents around the care of their children.
We helped fund much of the early stage research which is now being commercialised by Kitea Health. The technology has many other potential applications – not just for hydrocephalus and brain pressure monitoring – but more broadly in the remote monitoring of pressure in other chronic conditions, e.g. heart failure. The potential application of this breakthrough, and related technology, is massive.
Trends in autism prevalence and health service use in Aotearoa
Dr Nicholas Bowden, University of Otago
Autism is a neurodevelopmental difference that influences the way a person communicates, interacts, and experiences the world. International prevalence estimates suggest that 1 in 36 children are Autistic, but there are no official prevalence estimates in Aotearoa New Zealand.
Studies show that Autistic youth (ages 0-24) often have higher mental and physical health needs. However, there is a lack of research in Aotearoa New Zealand on how Autistic youth use healthcare services, which highlights the need for more studies to better understand and meet their healthcare needs.
These studies by Nick Bowden and his team will be used to inform the co-design of an evidence-based policy brief. In turn, this will provide policymakers with concise, well-researched recommendations to inform decision-making and promote effective policy solutions for the improved provision of healthcare for Autistic youth.
Helping to reduce the negative health impacts of rugby
Professor Nick Draper, University of Canterbury
Rugby Union is a popular contact sport played by 7.7 million players in 129 countries. About 160,000 New Zealanders play every season, including around 25,000 high school students. Because rugby involves a lot of physical contact, players face a higher risk of injuries compared to non-contact sports.
To understand concussions better, Dr Nick Draper and his team are looking closely at how players collide during the game, with a special focus on girls who play rugby. They are also testing special headgear approved by World Rugby to see if it can reduce the impact of collisions and lower the risk of injury.
This research is crucial to improve the understanding of concussion injuries in contact sports, especially rugby, and find ways to make playing safer.
Developing a mindfulness treatment for children with ADHD (attention deficit disorder)
Dr Mairin Taylor, University of Canterbury
ADHD is a common and debilitating neurodevelopmental disorder that affects 5 to 10% of New Zealand children. It is associated with higher rates of mood disorders, anxiety disorders, defiance disorders, risk-taking behaviour, and criminal offending.
Dr Mairin Taylor and her team will adapt an established mindfulness programme (MyMind) into a proposed ADHD treatment programme called MindKiwi. Their work will adapt a Kaupapa Māori framework – including Te Reo Māori and Tikanga principles – and once successfully adapted, the research team will examine its effectiveness with New Zealand children.
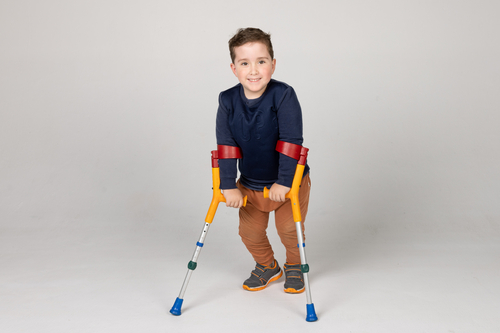
Benjamin was diagnosed with Spina Bifida Myelomeningocele and Hydrocephalus at his Mum Catherine’s 20-week antenatal anatomy scan. The family knew they had a battle on their hands but were determined to do everything they could for their little boy.
Ben and Mum qualified for a ground-breaking fetal surgery in Brisbane, Australia (Mater Mother’s Hospital) to help close the opening in his spine. At 24 weeks gestation, he was the first unborn kiwi and 3rd overall in Australasia to have this surgery.
Due to some complications post-surgery, Benjamin was born at 33 weeks gestation. In the first week of his life, he had an MRI scan and a very large fluid-filled cyst called a syrinx was found in his neural tube in his spine. Untreated this may have caused tetraplegia so a ventriculoperitoneal shunt (VP shunt) was inserted in his brain to relieve the pressure of the syrinx. Since then he has had three shunt revision surgeries, a decompression, and a syringo arachnoid shunt placement.
During the early stages of his diagnosis in pregnancy, Ben’s family were told he would potentially not have any movement of his legs. However, Benjamin can walk with a walker and crutches and is cognitively meeting all his milestones. He is such a happy, bubbly and gentle boy.
“He loves playing with his older brother Jackson. Benjamin is a little miracle and we are so lucky to have him,” Catherine says.
3 Active Neurological and Neurodevelopmental Disorders projects
-
Dr N. BowdenTrends in autism prevalence and health service use in AotearoaAwarded $124,442Neurological and Neurodevelopmental Disorders
-
Professor N. DraperHelping to reduce the negative health impacts of rugbyAwarded $124,900Neurological and Neurodevelopmental Disorders
-
Ass Prof L. McLayTelehealth for learning by children on the autism spectrumAwarded $499,940Neurological and Neurodevelopmental Disorders

Help fund researchers like Simon.
Every cent helps, no matter how small.
Big Research
We are currently supporting over $16 million of child health research projects.
Learn more-
Preterm Health
4 Active projects$464.8K -
Childhood Cancers
2 Active projects$3.2M -
Maternal and Infant Conditions
8 Active projects$751.4K -
Rheumatic Heart Disease
6 Active projects$2.8M -
Childhood Development & Sensory Studies
1 Active project$228K -
Neurological and Neurodevelopmental Disorders
3 Active projects$749.2K -
Endocrinology, Metabolism & Nutrition
2 Active projects$125K -
Mental Health and Wellbeing
9 Active projects$1.2M -
Oral and Dental Disease
2 Active projects$151K -
Genetic Conditions and Rare Disorders
3 Active projects$801K -
Respiratory Conditions
5 Active projects$862.6K -
Infectious Disease
2 Active projects$219.7K -
Gastrointestinal Conditions
1 Active project$600K



